Baseline characteristics
Clinical picture and comorbidities
PCS Patients (36% women) were referred to rehabilitation with a mean age of 50.2 ± 10.7 years (female, 47.1 ± 12.7; male, 52.0 ± 9.1; Fig. 1) and a mean Body Mass Index (BMI) of 30.4 ± 5.9 kg/m2 (female, 28.7 ± 6.1; male, 31.3 ± 5.6). The mean time interval between the first infection and start of medical rehabilitation was 262.0 ± 123.8 days (female, 285.5 ± 140.6 days; male, 248.8 ± 112.0 days; p = 0.110). No significant differences between female and male patients were detected with respect to lead symptoms (all p ≥ 0.458). Overall, fatigue/exercise intolerance was the most prevalent lead symptom observed in 81.4% of patients, followed by shortness of breath (74.5%), and cognitive dysfunction (52.4%) (Fig. 1). During the acute phase of infection, 72.4% of patients had received ambulant care or acute care at home (female, 80.7%; male, 67.7%), while 27.6% of patients required in-hospital care (female, 19.3%; male, 32.4%; p = 0.092). The need for ventilation during hospitalization was lower in women (not significant, p = 0.096). Patients reported a high frequency of endocrine, nutritional, and metabolic disorders, as well as circulatory system disorders (Table 1), the latter being more frequent in men (p = 0.031). Accordingly, medication profiles exhibited variations between female and males. Results of blood analyses were within the reference range (data not shown). Overall, 33.1% were ever smoker (female, 28.8%; male, 35.5%). No correlations between time after acute infection and baseline exercise capacity, pulmonary function and perceived disease burden were detected (Additional file 1: Figure S1).
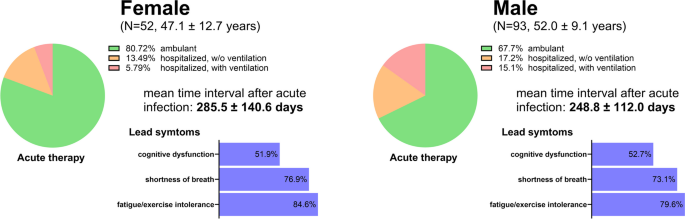
Characteristics of female and male patients with Post-COVID-19 syndrome (PCS). PCS patients were referred to rehabilitation 262.0 ± 123.8 days after acute infection (no difference between women and men, p = 0.110). At admission, affected women were significantly younger than men (p = 0.018). During the acute phase of infection, women had less often been hospitalized (p = 0.092), and need for ventilation during acute care was lower (p = 0.096). Women and men did not differ in lead symptoms at the onset of rehabilitation (all p ≥ 0.454; multiple naming possible). Data is presented as mean ± SD or %. Between-group comparison was performed using unpaired two-sided t-test or Chi-square test for categorical variables
Exercise capacity and pulmonary function
At baseline, PCS patients exhibited a significant limitation in submaximal and peak exercise capacity at 12.3 ± 3.4 ml/min/kg and 18.0 ± 4.3 ml/min/kg equal to 49.9 ± 12.3% and 73.6 ± 15.0% of predicted reference, respectively. Of note, women presented with a significantly higher relative peak exercise capacity (VO2, ml/min/kg) of 82.0 ± 14.3%, compared to men with 68.8 ± 13.3% (p ≤ 0.001; Fig. 2; Table 2). In addition, women had significantly higher heart rate and O2-pulse at submaximal exercise, as well as higher peak heart rate, O2-pulse and respiratory minute ventilation and reached higher workload compared to men using relative reference values for adjusted comparison (all p ≤ 0.018). Restrictions in pulmonary function were mainly reflected in reduced expiratory flow variables (Table 3) and maximum inspiratory pressure (MIP). Men exhibited higher values for FEV1, FEV1/VC, PEF and maximum expiratory flow (MEF25-75) (all p ≤ 0.038) and lower vital capacity (VC) at baseline compared to women (p = 0.019). The threshold for inspiratory weakness (≥ 80 cmH2O) was reached in 66.2% of PCS patients with significant difference between women and men (female, 78.8%; male 59.1%; p = 0.038).

Female and male patients with Post-COVID-19 syndrome (PCS) differ in submaximal and maximal exercise capacity. Female PCS patients (n = 52) showed higher relative submaximal and maximal exercise capacity determined by oxygen uptake (cardiopulmonary exercise testing, CPET) compared to male PCS patients (n = 93) at start of rehabilitation. While females and males showed an overall improvement of exercise capacity in response to rehabilitation (significant time effect), female patients showed a significantly greater improvement in submaximal workload (watt @ VT1) compared to males (significant time × group interaction). Pre: at admission, Post: at discharge. Data is presented as mean ± SD, each data point represents an individual measurement. Differences between groups over time were performed using two-way repeated measures ANOVA of percent predicted values (reference values) corrected for sex, age and body surface area. * p ≤ 0.05, ** p ≤ 0.01, *** p ≤ 0.001, **** p ≤ 0.0001
Perceived disease burden and workability
PCS patients showed overall high levels of fatigue (MFI-20 score, 69.2 ± 13.2) and low health-related quality of life for both, the physical (31.5 ± 8.3) and mental (36.2 ± 11.8) SF-36 components at admission (Fig. 3). Fatigue showed considerable negative correlations with exercise parameters peak workload (p = 0.040, r = -0.179), VE (p = 0.027, r = -0.192) and tidal volume (p = 0.041, r = -0.178), as well as pulmonary function (FEV1/VC, p = 0.007; r = -0.235; PEF, p = 0.032, r = -0.186; MEF50, p = 0.013; r = -0.215) (Additional file 1: Figure S1). Overall workability was low (22.3 ± 7.8) with a median maximum incapacity for work of 99 days during the last 12 months, while wellbeing was significantly reduced. Notably, female patients demonstrated significantly higher levels of fatigue and lower ratings of wellbeing at baseline (MFI-20 score, 73.4 ± 12.5; WHO-5 score, 7.0 ± 5.0) compared to males (MFI-20 score, 67.0 ± 13.1; WHO-5 score, 9.5 ± 5.2, both p ≤ 0.027). Of note, ~ 60% of female patients had an MFI-20 score above 70 (n = 29).
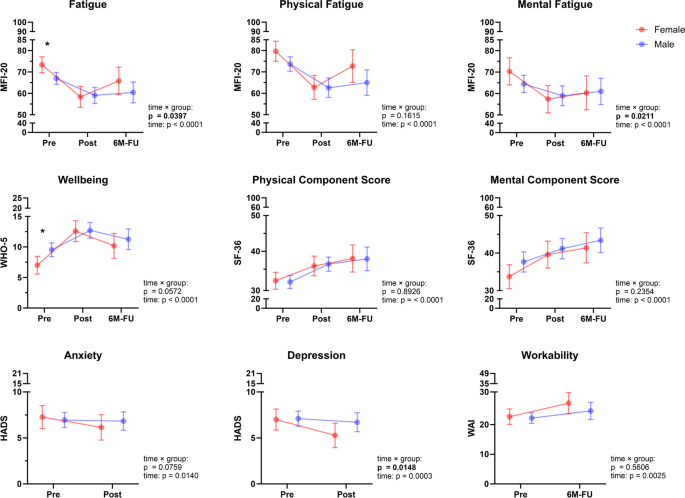
Female and male patients with Post-COVID-19 syndrome (PCS) differ in disease perception. Women presented with significantly higher levels of fatigue and lower wellbeing compared to men. While subjective impact of disease was significantly improved in all domains over time (time effect), female PCS patients showed a significantly different time course for development of fatigue and depression (significant time × group interaction). Disease perception was assessed by validated questionnaires at admission (Pre), discharge (Post) and after 6-months (6 M-FU). Anxiety, depression (pre, post) and workability (pre, 6 M-FU) were only assessed twice. Questionnaires were completed at admission (N = 132), discharge (N = 128) and 6-month follow-up (N = 89). Data is presented as mean and 95% CI. Differences between groups over time were performed using mixed-effects model. MFI-20, Multidimensional Fatigue Inventory; WHO-5, Well-being; SF-36, Health-related quality of life; HADS, Hospital Anxiety Depression Scale; WAI, Workability Index. * p ≤ 0.05
Rehabilitation and rehabilitation outcomes
The overall mean length of inpatient rehabilitation was ~ 4 weeks (28.8 ± 6.1 days) with no significant difference between female and male patients (p = 0.401). During rehabilitation, patients performed a mean of 12 exercise-based (active) therapy sessions per week with a participation rate of 91.4 ± 13.6% (female 90.2 ± 12.1%; male, 92.0 ± 14.5%; p = 0.437). Of these, 3–4 sessions were ergometer training, in which female and male patients were able to increase their workload equally by ~ 10%. Occurrence of post exercise malaise (PEM) was very low with only 3 reported cases. Overall, patients performed 1586.8 ± 479.4 min of exercise (cardio, 1248.3 ± 398.4 min; strength, 338.5 ± 145.3 min) equal to 107.0 ± 37.0 METs (female, 100.2 ± 36.2 METs; male, 110.7 ± 37.2 METs; p = 0.103), which were comparable between female and male patients in terms of cardio METs (female, 81.6 ± 31.5 METs; male, 90.4 ± 34.1 METs; p = 0.131) and strength METs (female, 18.6 ± 9.5 METs; male, 20.4 ± 7.9 METs; p = 0.262). In addition, patients performed ~ 8 educational, counselling, and occupational therapies and ~ 3 relaxation therapies per week.
During rehabilitation, an overall improvement of physical exercise capacity was detected at submaximal and peak load (all p ≤ 0.001; Fig. 2) in that peak oxygen uptake increased by 1.1 ± 2.9 ml/min/kg (4.6 ± 12.2% reference) while oxygen uptake at VT1 and VT2 increased by 1.2 ± 3.2 ml/min/kg (4.0 ± 11.0%) and 0.9 ± 3.1 ml/min/kg (+ 3.2 ± 11.9%), respectively. In addition, pre-exercise resting heart rate was significantly lower, while O2-pulse, respiratory minute volume and tidal volume at both submaximal and peak exercise increased significantly (all p ≤ 0.041; Table 2). Notably, and despite male patients starting at a lower level of cardiopulmonary exercise capacity, female patients showed greater improvements for workload at VT1 (time x group interaction, p = 0.0262) and a tendency to greater improvements in oxygen uptake (not significant, p = 0.079). Since men and women were not matched for cardiopulmonary exercise capacity, ANCOVA with baseline values for oxygen uptake as covariates was performed. This analysis suggested that female and male patients differed significantly in improvement of oxygen uptake at VT1 and peak load (both p ≤ 0.013). In addition, female patients showed higher improvements in respiratory minute ventilation at submaximal exercise (female, + 4.6 ± 8.4%; male, + 0.7 ± 8.8%; time x group interaction, p = 0.011). Application of more stringent criteria for maximal exercise testing (RER ≥ 0.95 for both CPETs, N = 128) revealed similar results. Responder analysis suggested that female and male patients responded equally to exercise-based rehabilitation at submaximal load (female, 67%; male 59%, p = 0.331) and at peak exercise (female, 60%; male, 58%; p = 0.856). Analyses of pulmonary function revealed an overall improvement for peak expiratory flow of 0.5 ± 2.0 l/s equal to 6.0 ± 23.8% (p = 0.005). Notably, female patients showed greater improvements for FEV1/VC compared to men (female, 4.8 ± 14.0; male, -1.0 ± 15.2; time x group interaction, p = 0.027), however, adjustment for baseline values did not confirm this difference (p = 0.590). Overall, MIP was significantly increased from 61.1 ± 28.1 cmH2O to 86.8 ± 32.6 cmH2O (p < 0.001; Fig. 4) with no significant difference between female and male patients (p = 0.865). However, 53.8% of female patients and only 28.0% of male patients were discharged with inspiratory weakness (≥ 80 cmH2O) (p = 0.004). Of note, patients were able to reduce their body weight by ~ 1.5 kg during rehabilitation (p < 0.001).
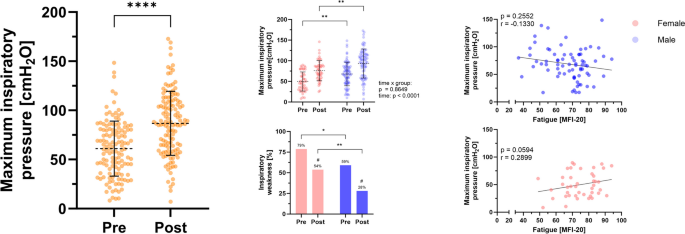
Patients with Post-COVID-19 syndrome (PCS) showed improved maximum inspiratory pressure (MIP) in response to rehabilitation. MIP was assessed at admission (Pre) and discharge (Post). Inspiratory weakness (MIP ≤ 80 cmH2O) was detected in 66.2% of PCS patients at admission and 37.2% of PCS patients at discharge, differing significantly between female and male patients. In female patients, higher MIP was associated with higher fatigue, while male patients showed lower MIP with decreasing fatigue. Data is presented as mean ± SD, each data point represents an individual measurement. Differences between groups over time were performed using two-way repeated measures ANOVA. Between-group comparison was performed using Chi-square test. Within-group comparison was performed using Mc-Nemar-Test. Correlations were performed using Spearman rank correlation. * p ≤ 0.05, ** p ≤ 0.01, **** p ≤ 0.0001, # Significantly different from Pre to Post (p ≤ 0.001)
In terms of disease perception, patients demonstrated improvements in fatigue, health-related quality of life, including the subcategories physical and mental component as well as wellbeing, depression and anxiety (all p ≤ 0.014; Fig. 3). Notably, female patients showed greater improvements in overall fatigue (female, -16.0 ± 15.8; male -7.5 ± 14.1), mental fatigue (female, -14.8 ± 17.6; male, -5.4 ± 13.2) and depression scores (female, -1.7 ± 3.8; male, -0.3 ± 2.5) compared to males (all time x group interaction: p ≤ 0.040). Of note, differences between female and male patients in improvement of disease perception, as well as exercise capacity and pulmonary function (except FEV1/VC) were independent of age, baseline body mass index, comorbidities and baseline values.
Maintenance effects after 6 months
To record the medium-term effects of rehabilitation on disease perception and workability, patients were asked to fill out questionnaires after 6 months. Health-related quality of life as well as overall and mental fatigue remained unchanged compared to discharge, while patients showed a significant re-increase of physical fatigue (+ 4.6 ± 20.9; p = 0.032, 6 M-FU vs. post), with greater worsening in women (female, + 9.4 ± 23.7; male, + 1.7 ± 18.6; not significant, p = 0.129). In addition, wellbeing significantly decreased after discharge (-1.9 ± 6.0; p = 0.007) while workability showed an increase from admission to 6-months follow-up (p = 0.003) with no significant differences between men and women.
link

