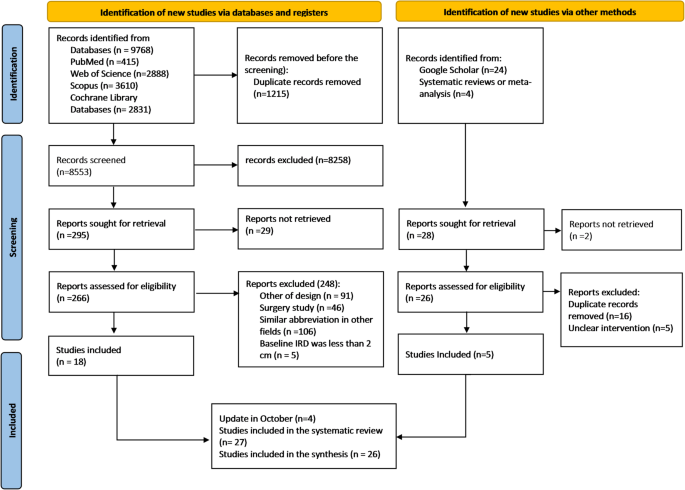
Study selection and General characteristics
The researchers found 27 RCTs out of 9,768 reviewed studies (Fig. 1). After removing duplicates, the search strategy yielded 8,553 records. Screening titles and abstracts identified 8,258 irrelevant hits. The remaining 266 full-text articles were assessed, and 27 studies met the inclusion criteria (see Appendices 2- Table S2, S3, 16- Table S31, S32, and Fig. 1). Of these, one study was not included in the main network of this quantitative synthesis due to the inconsistency of its intervention with other studies. The number of participants was 1340, and their age, BMI, and baseline IRD were 29.92, 25.26, and 28.21 mm, respectively (Table 1). In the data extraction process, we identified the number of participants in the intervention groups: physical agents (n = 43)10,11,13,29,31,34,48,49,50, exercise therapy (n = 574)5,8,13,18,19,23,24,25,26,32,33,51, mind–body practices (n = 18)27,35, different types of abdominal belts and tapes (n = 135)3,8,9,20,25,28, exercise therapy combined with physical agents (n = 338)10,11,13,29,34,48,49,50, exercise therapy combined with belts (n = 86)3,8,29,30,50, and no treatment (n = 146)3,5,13,19,25,27,28,51. The characteristics of all included studies are detailed in Appendix 4a- Table S6.
Risk of bias assessment
The results of the RoB2 assessment are shown in Fig. 2. Also, the results of the risk of bias assessment (e.g., supporting reasons, etc.) for each study based on the items of the Cochrane RoB tool version 2 were represented in Appendix 3- Figures S1, S2. Considering the overall (n = 27) risk of bias across studies, 62.96% of trials were exposed at a low risk of bias (n = 17), 29.63% at a high risk of bias (n = 8), and 7.40% of trials at unclear risk of bias (n = 2).
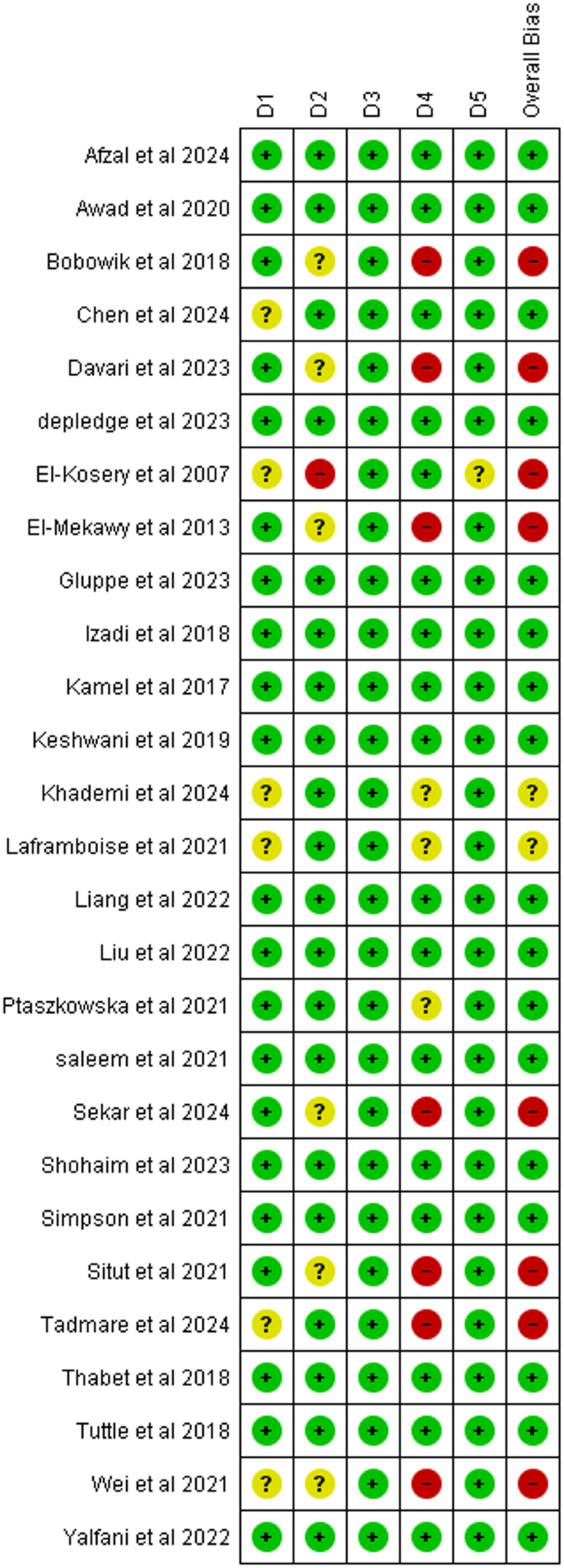
Summary of all risk-of-bias articles. D1, randomization process; D2, deviations from the intended interventions; D3, missing outcome data; D4, measurement of the outcome; D5, selection of the reported result.
Quantitative synthesis
Transitivity, heterogeneity, and inconsistency
No significant concerns were identified regarding the violation of the transitivity assumption in terms of clinical and epidemiologic features for participants of RCTs who were included in the NMA. There was only a slight concern about the duration of the interventions and the postpartum timing, which was resolved by subgroup analysis (Appendix 10- Table S17, Figure S8).
The heterogeneity of the studies indicated that the evidence was generally homogeneous (I2 = 26.80%, p = 0.1862, tau2 = 1.718). In two specific comparisons of NMES + TCME/TCME and TrAS/RL, the I2 was calculated to be 56.89% and 3.84%, respectively, suggesting probable superficial differences between studies in these cases. The inconsistency of the network evidence analysis revealed that the overall structure of the network was favorable in terms of consistency, with no significant difference between direct and indirect evidence (p = 0.1606). The global test of Design-by-Treatment Interaction confirmed that the overall network results were reliable and that there was no significant inconsistency in the association between interventions (p = 0.2029, tau2 = 2.953). Closed-loop analysis demonstrated that no significant inconsistency was observed in any comparisons, indicating both the stability of the combined results and the consistency of direct and indirect evidence in the meta-analysis network (p > 0.05). While this could suggest the absence of statistical heterogeneity among the studies in those comparisons, in this study, it was primarily due to the limited number of studies available for pairwise comparisons. To achieve stable estimates, at least 3 to 4 independent studies are needed in each comparison, which, in the present study, we faced this limitation due to the reduction of studies related to DRA therapeutic interventions. Finally, it is recommended to refer to Appendix 11- Tables S18, S19 for more complete information.
The results of networks
After the analysis of interventions, there were two separate sub-networks and the main network consisted of 26 studies. From 27 studies, the number of pairwise comparisons in the NMA was 42, and there were 31 treatments. The one study was a comparison of AB + LSE / Plank + AB + LSE from Awad et al.30, which was excluded from NMA. The direct and indirect comparison of treatments is shown in the league table (Appendix 9- Table S16) and forest plot (Appendix 8- Figure S7). The league table is a square matrix showing all pairwise comparisons in a network meta-analysis. Mean differences and their confidence intervals are provided in Appendices 7- Figure S3, S4, S6 and 13a-Figure S12, S13, S14 and 13b- Figures S15 to S20 to facilitate comparisons against the minimal clinically important difference (MCID) thresholds for IRD measurements (Table 3). On the other hand, the additive network meta-analysis model was applied for comparisons of treatments versus RL (no-treatment), and these analysis results were reported in Appendix 7- Table S15.
Network meta-analysis of IRD
26 out of 27 studies constituted an intervention treatment network for DRA. The nodes for the DRA analysis were defined at the level of the rehabilitation methods. Each single or combined treatment was a separate node, and the researchers indicated each of them with one color. Different routes of administration for the same interventions (or combination) were merged into the same node. The Network color information is available in Table 2. Based on the results of this NMA, the largest node belongs to RL, which means that most treatments have formed a network with this variable. The RL is a “no treatment” and most of the interventions were compared with it in this NMA. After that, the other big node belongs to the TCME intervention. This is a traditional exercise in physical therapy and most RCTs compared the newest treatments versus it. In the end, the “TrAS” method, as the last big node of this network graph, is an exclusive exercise method for transverse abdominal (TrA) muscle practice that some therapists use. As it is clear, some treatments formed closed loops with them, and the size of these nodes indicates the number of repetitions in the NMA. Figure 3 shows forming loops in the network graph.
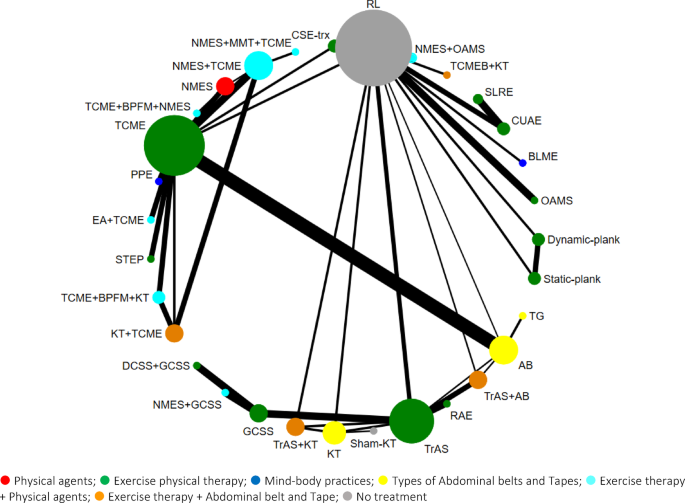
Treatment network graph for DRA. The node size is proportional to the number of RCTs in each intervention, and the line width is related to trials directly comparing the two interventions. colors refer to types of interventions.
The effect size of the treatments in this study is measured based on minimal clinically important difference (MCID) thresholds. According to the study of Mota et al. (2018), the MCID of IRD is approximately between 5 and 10 mm (Appendix 6- Tables S10, S11)5,41. Thus, the mean difference observed in the studies pre- and post-intervention is quantified using the 95% confidence interval and the MCID, ensuring a robust assessment of the clinical relevance of treatment effects (Table 3). The results of pairwise comparisons between treatment interventions are also presented in the form of a league and NMA tables, including the mean difference in effectiveness between the two treatments and the 95% confidence interval. The league table allows for direct assessment of the observed differences between the interventions and helps to understand the extent to which each treatment is more effective than the others. Examination of the values presented in the table indicates that some interventions had more significant effects than others, which can be taken into account in clinical decision-making. Their full details are provided in Appendix 9- Table S16. In the analysis of the results based on the interpretation of GRADE confidence coefficients for each pairwise comparison, as well as the clinical interpretation of the treatment effect in pairwise comparisons aimed at reducing IRD, it was observed that the greatest effect was in the comparison of TCMEB + KT versus RL (MD = –26.25). However, due to its low confidence, this result should be interpreted with caution. In contrast, the comparison of CSE-trx versus RL (MD = –25.14) was assessed with high confidence. Additionally, the comparisons of TCME versus RL (MD = –15.37), TCME + BPFM + NMES versus NMES (MD = –11.08), and REA versus TrAS (MD = –10.47) were also reported with high confidence. Meanwhile, the comparison of AB versus RL (MD = –10.32) showed moderate confidence, while the comparison of RL versus TrAS (MD = –10.15) was interpreted with low confidence. See Appendix 6- Tables S10, S11 and 14- Table S30 for further comparisons. According to Fig. 4, In the forest plot of DRA based on MCID threshold (All treatments Vs RL), it seems that the TCMEB + KT (SUCRA = 0.96, MD = -26.25)8, TCME + BPFM + NMES (SUCRA = 0.95, MD = -25.94)10, the CSE-trx (SUCRA = 0.94, MD = -25.25)5 and the NMES + MMT + TCME (SUCRA = 0.92, MD = -24.62)31 treatments versus the RL reduced the DRA more than others. It should be noted that exercise, physical therapy and physical agents were a main part of these treatments. Moreover, the DCSS + GCSS (SUCRA = 0.25, MD = -3.17)26, the Dynamic-plank (SUCRA = 0.23, MD = -2.60)32, the KT (SUCRA = 0.18, MD = -1.48)25,28, and the Static-plank (SUCRA = 0.17, MD = -1.10)32 indicated that they have a minimal effect on DRA than other interventions. On the other side, four interventions namely the GCSS (SUCRA = 0.11, MD = 0.28)26,33,48, Sham-KT (SUCRA = 0.10, MD = 0.52)28, CUAE (SUCRA = 0.09, MD = 1.00)12,19, and the SLRE (SUCRA = 0.02, MD = 3.86)12 were the weakest of these treatments, and not only did DRA not improve, but it seems they also caused that worse. Besides, there was no statistically significant difference between direct and indirect estimates of DRA (Appendices 7- Table S15 and 8- Figure S7).
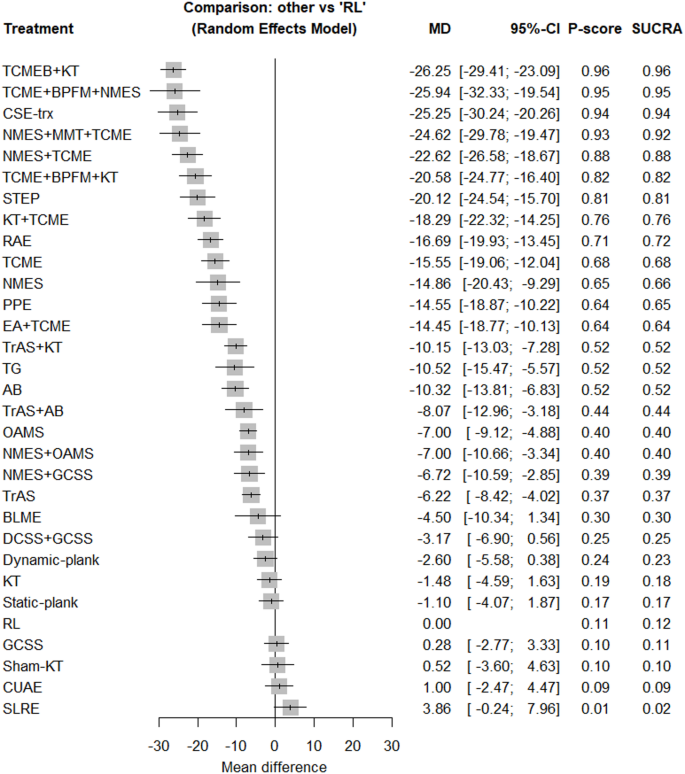
Forest plot- the network ranking of treatment methods in the DRA based on P-score, Confidence interval (CI) and Mean difference (MD). For Abbreviations, refer to Table 2.
The intervention duration subgroup
In the intervention duration subgroup, studies were divided into two groups above (22 studies) and below (5 studies) 18 sessions8,11,28,29,31. However, the network was formed only for interventions above 18 sessions, with 40 comparisons and 27 treatments (Appendix 13a). Based on the results of this NMA, the largest node belongs to RL. After that, the other big node belongs to the TCME intervention. In the end, the TrAS is the last big node of this network graph. As it is clear, some treatments formed closed loops with them, and the size of these nodes indicates the number of repetitions in the NMA. Appendix 13a shows the formed loops in the network graph.
In the forest plot of long-term interventions for improving DRA, it seems that the TCME + BPFM + NMES (SUCRA = 0.98, MD = -25.14)10, CSE-trx (SUCRA = 0.97, MD = -25.25)5, NMES + TCME (SUCRA = 0.91, MD = -21.89)29,31,34,49 and TCME + BPFM + KT (SUCRA = 0.89, MD = -21.17)50 treatments versus the RL reduced the DRA more than others. It should be noted that exercise, physical therapy and physical agents were a main part of these treatments. Moreover, the DCSS + GCSS (SUCRA = 0.26, MD = -2.94)26, the Dynamic-plank (SUCRA = 0.24, MD = -2.60)32, the KT (SUCRA = 0.18, MD = -1.24)25,28, and Static-plank (SUCRA = 0.16, MD = -1.10)32 indicated that they have a minimal effect on DRA than other interventions. On the other side, three interventions, namely the GCSS (SUCRA = 0.09, MD = 0.51)26,33,48, CUAE (SUCRA = 0.08, MD = 1.00)12,19, and SLRE (SUCRA = 0.01, MD = 3.86)12 were the weakest of these treatments, and not only did DRA not improve, but it seems they also caused it to worsen. Moreover, there was no statistically significant difference between direct and indirect estimates of DRA (Appendix 13a- Figures S12, S13, S14).
Five out of 27 studies evaluated improving the IRD with interventions under 18 sessions8,11,28,29,31. Due to the small number of studies, quantitative analysis was not performed and there is no certainty to compare short-term and long-term interventions. However, their results of IRD improvement were presented as follows: EA + TCME (MD = -6.41 ± 3.82) from Liu et al.11, TCMEB + KT (MD = -18.65 ± 4.80) from Bobowik et al.8, NMES + TCME (MD = -13.8 ± 3.49; -11 ± 4.85) from Chen et al.31 and Situt et al.29, NMES + MMT + TCME (MD = -15.8 ± 7.07) from Chen et al.31, KT + TCME (MD = -2.99 ± 4.99) from Situt et al.29, KT (MD = -2 ± 1.42) from Ptaszkowska et al.28.
The IRD timing of the postpartum subgroup
The timing postpartum, which was the second subgroup of studies, was divided into three groups: immediate time (< 6 weeks)3,8,9,20, early time (6 weeks to 6 months)5,10,12,13,23,25,26,29,30,31,32,33,34,35,48,49,51, and late time (> 6 months)11,18,19,27,28,50. This indicates a difference in the time intervals for treatment initiation and outcome assessment (Appendix 13b). This subgroup analysis was conducted to evaluate the impact of intervention timing as a determinant of treatment effect size, while also distinguishing the intervention effects from the natural postpartum spontaneous recovery process. The findings indicated that the majority of treatments fell within the ‘early time’ category, signifying that interventions were generally administered within a moderate post-initiation timeframe, and their effects subsequently assessed. However, due to limited evidence and a lack of common pairwise comparisons across all three temporal groups, no conclusive insights could be drawn regarding the influence of intervention timing on treatment efficacy. In the analysis of the Immediate time, the comparison between TCME and RL yielded a P-score of 1.00 with a mean difference (MD = -13.10), indicating a definite clinical effect on IRD, and other treatments were possible effects. In the Early time subgroup, researchers observed a spectrum of effects from definite to probable, ranging from TCME + BPFM + NMES to TrAS + KT treatments. Finally, in the Late time subgroup, due to the absence of RL in pairwise comparisons, all treatments were evaluated against TCME, so they can not be compared to the two other groups. For a comprehensive overview, including NMA results for subgroups, network structures, ranking forest plots, and pairwise treatment comparisons, please refer to Appendix 13b- Figures S15 to S20.
Qualitative synthesis of outcomes
The qualitative report of the studies regarding mean and standard deviation pre- and post-interventions of IRD, which includes information on the observed changes, can be reviewed in full in Appendix 4b- Table S7. Also, 20 out of 27 studies assessed secondary outcomes related to DRA3,5,10,11,12,18,19,20,23,25,26,28,29,31,34,35,48,49,50. Since the reporting of secondary outcomes was heterogeneous and a small number in RCTs, thus, these data could not be quantified. The secondary outcomes assessed by RCTs were QoL, Disability, abdominal strengthening and endurance, core muscle thickness, postural stability, lumbopelvic control and proprioception, back pain, etc., that were reported as a qualitative synthesis of findings in Appendix 4c- Table S8.
Sensitivity analysis
To assess the impact of high-risk studies on the overall results, a sensitivity analysis was performed by excluding these studies. After excluding high-risk studies, the heterogeneity (I2) value decreased from 26.80% to zero, indicating an improvement in the consistency of the data in the meta-analysis network model. However, this change was minor and did not have a significant impact on the overall results, indicating the robustness and reliability of the analyses performed. Detailed details of this analysis are provided in Appendix 12- Figures S9, S10 and Table S20.
Certainty of evidence and publication bias
In the GRADE assessment, most comparisons in this analysis network were based on a single study, except for two comparisons, RL/TrAS and NMES + TCME/TCME, which involved two studies, which limits the analytical power and the generalizability of the results. Because of the absence of complementary data, a more precise evaluation of heterogeneity and inconsistency in these comparisons was not achievable. Therefore, the findings from these comparisons (54.77% high confidence, 30.96% moderate confidence, and 14.28% low confidence) should be interpreted cautiously, and further research is advised to confirm or refute these results. Although relying on a single study may have limitations regarding generalizability, most comparisons were generally rated as moderate to high confidence due to well-designed and methodologically sound studies, low risk of bias, adequate precision (narrow confidence intervals), and close alignment with the research question. This suggests that despite being sourced from a single study in each comparison, the available evidence is of high quality. Hence, in the evidence analysis, 11 pairwise comparisons from two pilot studies were downgraded by one GRADE level due to limitations commonly associated with these types of studies (such as small sample sizes, preliminary experimental design, and the potential for greater imprecision). In other words, since these comparisons were based on pilot studies, they were reduced by one level according to the GRADE quality of evidence standard to reflect the possible weakening of the precision and generalizability of the results. In the GRADE table report, in the “Overall confidence” column for these 11 comparisons, the quality was specifically downgraded from high to moderate or moderate to low, while other similar comparisons based on RCT studies may be of higher quality. So, the GRADE judgments are reported in Appendix 14- Table S30 for the IRD network meta-analysis. As well as, the authors applied the Egger test and the funnel plot to assess publication bias (p = 0.552), and their result was reported in Appendix 15- Figure S21 and Fig. 5.
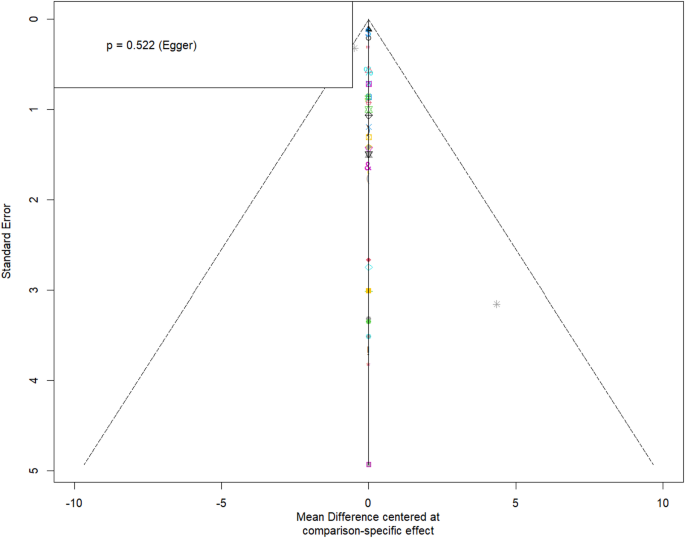
Egger funnel plot of DRA designed by R software.
link